The first Wellington-Dufferin-Guelph Board of Health meeting for 2021 offered some hope for the future even if it wasn’t an immediate hope. With vaccine delays out of her control, Medical Officer of Health Dr. Nicola Mercer focused on the swift delivery of what vaccines have been received, and the fact that it looks like the virus has peaked in Guelph and area for this second wave.
Mercer reported that public health has handed out 6,553 doses of the COVID-19 vaccine from Pfizer. At a delivery rate of 2.512 per 100,000 people that puts Wellington-Dufferin-Guelph on par with the entire Province of Ontario in terms of rate of delivery despite the fact that they received their first vaccines three weeks later than other jurisdictions.
The bad news is that there’s not enough vaccines at the moment to continue to hand out first shots to phase one patients.
“We had to stop because literally we ran out of vaccines,” Mercer explained. “We had to stop all our clinics and hold the vaccine that we have and wait till we get a little bit more vaccine, which came in this week on Monday, so that we can have enough vaccine to give the second dose to all of those first doses.”
According to figures provided by Mercer, 3,055 of the vaccine doses handed out so far have been to residents of long-term care and retirement homes, while about 1,709 have to gone to healthcare workers in those homes. Another 1,589 shots went to healthcare workers in other settings like the hospital where there are frontline workers who have direct contact with COVID patients. The last 157 shots went to “essential visitors” at long-term care homes, a conceit to the fact that public health is trying to use every dose of the vaccine, which has to be administered to a patient once thawed or else go to waste.
“Once we’ve punctured a vial we have to use it within a very short time frame,” Mercer explained. “When we go into the settings where we are immunizing people and people decline a vaccine or don’t show up, if there are any spare doses then we try very hard to ensure that those doses end up in people who are next on the list, and essential caregivers in our long-term care and retirement homes are on the list to receive the vaccine.”
Mercer said that she is not expecting to receive any more doses of the vaccine until the week of February 15, but she added that all public health needs is the actual vaccine because they’re ready to move very, very quickly. She reported that all residents in long-term care have received their first does of the vaccine, and public health is on track to fully vaccine residents with their second doses by February 24.
“We have lots of plans underway for when we get vaccines, and I strongly believe it is possible and doable that we will have our vaccine coverage and we will get people immunized locally in a very short amount of time,” Mercer added.
The provincial guidelines for vaccine distribution require residents of long-term care, retirement homes, and high-risk healthcare workers be the first to get their vaccines followed by residents living in congregate setting, individuals receiving home or community care, and Indigenous communities. Phase two, which will work backwards from seniors over the age of 80 to people 65 and older is scheduled to begin in April, while everyone that wants a vaccine should be able to get a vaccine starting in June.
In the midst of this good news though, Dr. Mercer reminded that board that it could still be a long while before things get completely “back to normal.”
“As we reach a certain threshold then yes, we will be able to remove our face coverings and our masks someday, and we will be able to get a little closer than six feet but I’m not going to tell you to to stop washing your hands or using a hand sanitizer,” Mercer said. “I think those are going to be habits that we’re going to have to keep for a very long time.”
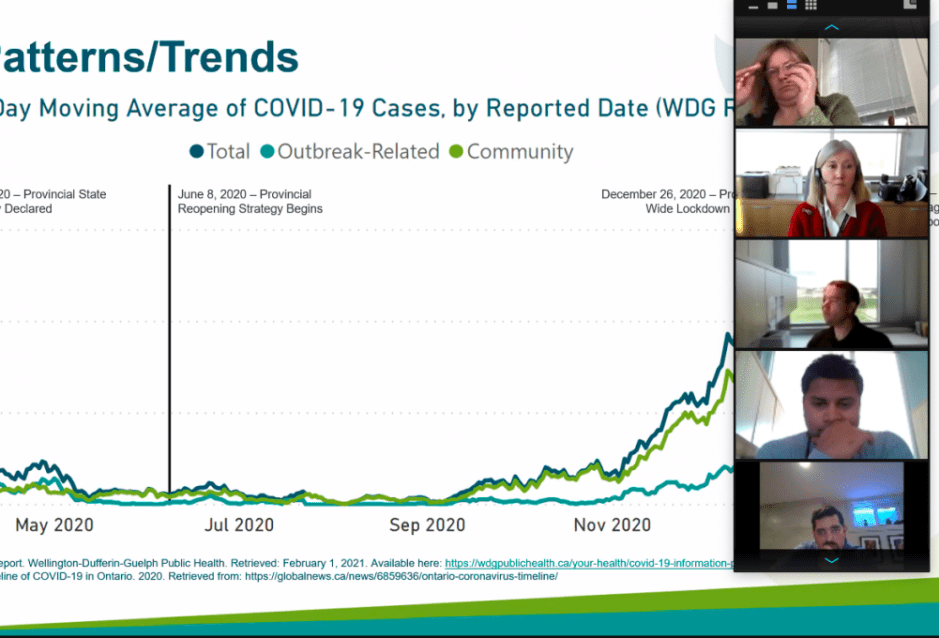
In terms of the COVID cases right now, public health staff noted that the surge of new cases of the virus peaked on January 9. The control threshold for the spread of the virus, meaning the point at which more extreme actions have to be taken, is 40 per 100,000, and that number on Wednesday was 81.6 per 100,000 according to the public health status board.
Still, Mercer drew the board’s attention to the mortality rate, where 89 per cent of the COVID-19 deaths in our area have been suffered by people over the age of 65; the other 11 per cent were people over 60 years of age. Mercer’s point is that while young people may not feel like they’re in much danger, the seniors in their life are in very pronounced danger if they catch COVID.
“The risk is not spread equally across our society, and some people are more likely to have bad outcomes than others,” Mercer said. “If you look at [these stats], it’s really obvious that the older you are, the more likely you are to have a risk of serious illness, and certainly you have a higher instance of dying.”